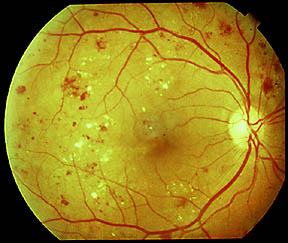
Retinal changes seen in special situations include the following: Optic nerve changes: Edema or, in later stages of optic neuropathy, optic disc pallor is seen. Follow-up scans show a resolution in increased central foveal thickness in the right eye (C) and symmetry of architecture with that of the left eye (D). 1: OCT scans show a slight increase in central foveal thickness in the right eye (A) as compared with the left eye (B). These findings are seen more as the severity of anemia increases.įigure 2. Vessel changes: Arteries are attenuated and pale, and veins are dilated and tortuous. When these are severe and located at the macula, macular star is seen. Hard exudates: These may be seen due to resolved retinal edema. Retinal edema: The microtrauma of the vessel wall secondary to raised transmural pressure leads to leakage. 6Ĭotton wool spots: Retinal nerve fiber layer infarction due to retinal hypoxia in anemia causes these superficial fluffy white lesions. 
The white centers in Roth spots can be due to inflammatory infiltrates, fibrin and platelets, neoplastic cells, or focal areas of ischemia. Rarely, blood may be present in the subhyaloid plane or in the vitreous. In a few cases, dot and blot hemorrhages in deeper retinal layers may be noted. Hemorrhages: Superficial, flame-shaped hemorrhages located in the nerve fiber layer are the most common finding in anemic retinopathy. Retinal changes common to all anemias include the following: 
Alternatively, vision loss may occur due to disc edema or optic neuropathy. At the macula, hemorrhages, edema, or hard exudates can cause impairment of vision. Rarely, loss of vision can be a presenting complaint, because most cases are asymptomatic. The clinical picture in D is the left eye.Īlong with systemic features of anemia per se, and in relation to the primary etiology leading to the anemia, ocular findings can be classified as features common to all anemias or specific features due to specific etiologies. On follow-up, the macular edema resolved in the right eye (C). 1: Fundus photos showing retinal edema in the patient’s right eye (A) as compared with the left eye (B). Hypotension may lead to optic neuropathy. Other factors implicated in the pathology are venous stasis, angiospasm, increased blood viscosity (myeloproliferative disorders), hypotension (following hemorrhage), etc. In many clinical situations, thrombocytopenia is associated with anemia, and that leads to defective coagulation and hemorrhages. Retinal hypoxia also leads to vascular dilatation increased transmural pressure owing to hypoproteinemia and microtraumas to the vessel walls, which cause retinal edema and hemorrhages. Anemia causes retinal hypoxia, which leads to infarction of the nerve fiber layer and clinically manifests as cotton wool spots. 3Ī variety of pathologic changes occurring due to and associated with anemia are implicated in the clinical features of anemic retinopathy. As the severity of anemia increases, the risk of retinopathy increases, particularly when the hemoglobin (Hb) level is below 6 gm/dL. 2 EPIDEMIOLOGY and PATHOGENESISĪnemia causes retinopathy in 28% of patients, especially when there is coexisting thrombocytopenia (38%). These were first described by Ulrich in 1883 in association with gastrointestinal hemorrhage. 1 In the eye, anemia can lead to transient retinal hemorrhages. A deficiency of vitamin B12 is known as pernicious anemia. Iron deficiency is the most common type of anemia.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
